October is Breast Cancer Awareness Month. Breast Cancer can be a massive and a startling topic, and is the most common form of cancer affecting Malaysian women. About one in 20 women in Malaysia are at risk of breast cancer.
One in 10 of all new cancers diagnosed worldwide each year is a cancer of the female breast, and it is the most common cancer in women in both developing and developed areas. It is also the principal cause of death from cancer among women globally.
According to the Malaysia National Cancer Registry Report (MNCRR) 2012-2016, roughly 34 women out of 100,000 got breast cancer from 2012 to 2016, compared to about 31 women from 2007 to 2011.
Men can also get breast cancer with a reported incidence of one percent, and thought to behave similarly in both genders.
Cancer support groups have great healing benefits to help patients, survivors and care givers cope and share individual experiences, and learn from one another within a safe environment.
Early screening and appropriate medical treatment can save lives. Don’t be afraid to ask questions from your doctors to better understand breast cancer and treatment options.
It is important to differentiate between myths and facts about breast cancer. In this article, Sri Kota Specialist Medical Centre’s Consultant Oncologist, Dr Malwinder Singh Sandhu addresses the subject and misconception; while Breast Cancer Welfare Association Malaysia (BCWA) President , Ms Ranjit Kaur shares the importance of support groups in relation to breast cancer support groups, role and benefits.
- Myth : A lump in the breast means you have breast cancer
Fact: Firstly, a lump in the breast doesn’t mean its cancer. Only 20% of breast lump are cancerous. The other 80% of lumps are benign (non-cancerous) such as cysts and fibroadenoma. Some lumps come and go during a woman’s menstrual cycle. You should be worried if the lump is hard, not moveable, and not smooth. That is why we advocate monthly self-breast examination.
Secondly, you can still get breast cancer without a palpable lump. This happens in early-stage cancers. This is another reason why regular screening mammogram is so important to detect early stage cancers.
- Myth: Women with breast cancer have a family history
Fact : Most women who have breast cancer have no family history of the same. However, women with a family history of breast cancer are in a higher risk group. There are only about 10% of individuals diagnosed with breast cancer have a family history of this disease.
- If you have a first degree relative with breast cancer: If you have a mother, daughter, or sister who developed breast cancer below the age of 50, you should consider some form of regular diagnostic breast imaging starting 10 years before the age of your relative’s diagnosis.
- If you have a second degree relative with breast cancer: If you have had a grandmother or aunt who was diagnosed with breast cancer, your risk increases slightly, but it is not in the same risk category as those who have a first degree relative with breast cancer.
- If you have multiple generations diagnosed with breast cancer on the same side of the family, or if there are several individuals who are first degree relatives to one another, or several family members diagnosed under age 50, the probability increases that there is a breast cancer gene contributing to the cause of this familial history.
- Myth: Breast cancer only affects older women
Fact : Breast cancer can affect women of any age. Although breast cancer most commonly affects women between 50-60 years old, it can also occur in women less than 40 years old and the elderly. About 26% of Malaysian women with breast cancer are below 45 years old and 3.9% occur in those above 75 years of age. However, studies have shown that elderly do just as well as younger women if they receive appropriate treatment. Therefore, age alone should not be a barrier to receiving treatment.
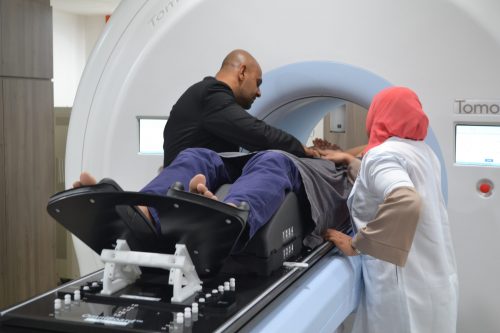
Studies have shown that elderly do just as well as younger women if they receive appropriate treatment.
- Myth: Hormone Replacement Therapy (HRT) does not increase the risk of breast cancer
Fact : Most types of HRT increase the risk of breast cancer. But the risk is higher for those using combined HRT, which uses both oestrogen and progestogen. Taking HRT for 1 year or less only slightly increases breast cancer risk. However, the longer you take HRT the greater the risks are, and the longer they last. The risk of breast cancer due to HRT can also vary from person to person. Things such as what age you are when you first start taking HRT, other medicines you may be taking, and your general health can impact the risk. People who begin HRT before or soon after the menopause may have a bigger risk than those who start HRT later.
- Myth: Breast cancer can be cured with new advanced treatment techniques
Fact : Breast cancer can only be cured if the cancer is detected early. If the cancer has spread to other organs the chance of cure diminishes. However, with newer technological advances such as targeted therapy and immunotherapy, we are able to treat cancer like any other chronic illness such as diabetes and hypertension. The survival for advanced stage breast cancer has increased over the years compared to 20 years ago.
- Myth: Mammograms prevent breast cancer in women
Fact: A mammogram is an X-ray of the breast. For many women, mammograms are the best way to find breast cancer early, when it is easier to treat and before it is big enough to feel or cause symptoms. Having regular mammograms can lower the risk of dying from breast cancer. Currently, a mammogram is the best way to find breast cancer for most women of screening age.
- Myth: Healthy diet prevent breast cancer
Fact : Eating more vegetables and fruits may work in several ways as part of an overall healthy eating pattern and lifestyle to reduce breast cancer risk. Excess body fat does increase risk for postmenopausal breast cancer. Therefore, substituting low-calorie vegetables and fruits for foods high in calories can help, because research strongly supports this key step in weight management. The strongest effects seem to come from reaching and maintaining a healthy weight, getting regular physical activity and minimizing alcohol consumption. For all these reasons, eating more vegetables does make sense as one part of an overall lifestyle to reduce breast cancer risk and promote overall health.
- Myth: Using antiperspirants and under – wire bras cause breast cancer
Fact : Antiperspirants and deodorants are safe to use every day and they don’t cause breast cancer. It is wrongly believed that aluminum and parabens in these personal care products are absorbed through the skin, or through cuts caused by underarm shaving, and cause breast cancer. Reputable organizations like the American National Cancer Institute, Cancer Research UK, the American Cancer Society and most other major authorities suggest the link between deodorant or antiperspirant use and breast cancer is unconfirmed, or simply a myth.
It is completely safe to wear a bra. There is no scientific evidence to link wearing a bra, the type of bra worn (under-wired or non-wired) or the length of time it is worn, with breast cancer risk. The authors of a new breast cancer study on post-menopausal women, funded by the US National Cancer Institute and published in the September 2014 issue of Cancer Epidemiology, Biomarkers & Prevention, said: “Our results did not support an association between bra wearing and increased breast cancer risk among post-menopausal women.”
- Myth: Birth control pills can cause breast cancer
Fact: Current or recent use of birth control pills (oral contraceptives) is linked to a slight increase in the risk of breast cancer. Studies show while women are taking birth control pills (and shortly after), their breast cancer risk is 20-30 percent higher than women who’ve never used the pill. However, this extra risk is quite small because the risk of breast cancer for most young women is low. So, even with a slightly higher risk from taking the pill, most young women are unlikely to get breast cancer. Once women stop taking the pill, their risk of breast cancer begins to decrease. Over time, risk returns to that of women who have never taken the pill.
- Myth: An injury to the breast can give rise to breast cancer
Fact : There’s no good scientific evidence that trauma, injury or a blow to the breast can cause cancer and there’s no good explanation for how an injury could cause cancer. Sometimes an injury can cause a non-cancerous (benign) lump known as fat necrosis. This is scar tissue that can form when the body naturally repairs itself. There’s no evidence to suggest that fat necrosis can increase the risk of cancer.
BCWA offers psychosocial peer (emotional and social) support as well as information for individuals affected by breast cancer enabling them to be better informed and to manage themselves during and after treatment. In BCWA, breast cancer survivors who have completed treatment are trained, certified and supervised to offer peer support to newly diagnosed breast cancer patients and their care givers.
Previously the support was given face-to-face but now with the Covid-19 pandemic, it is done online – voice call and WhatsApp messages. Group counselling is done online every 3rd Saturday, and we also have one educational session by an expert and a therapeutic session to help patients through recovery and rehabilitation.
- How important is it to have the support of others for breast cancer survivorship?
Peer support: The presence of a breast cancer survivor living a normal life, looking healthy after completing treatment is certainly a sense of motivation and encouragement for the new patient. The patient is meeting someone who has experienced a journey that the patient is just starting. The experience of the long term survivor creates validity for the patient that there can be life after breast cancer.
Having received training the peer volunteer is non-judgemental, a good listener, articulates effective coping strategies and enable positive coping skills in the patient. This form of support helps improve the quality of life of the patient.
2. Does recovery programs for patients and survivors help?
Having gone through the breast cancer experience myself, I can safely say that initially I was always drawn to be in the company of other breast cancer survivors who were supportive, understood how I felt and they made me feel motivated to pursue with my treatment and its challenges.
3. Does BCWA offer peer support for caregivers of cancer patients?
BCWA offers support to care givers by enabling them to be well informed and supporting them through their challenges and also helping them to understand the disease and its impact.
In fact, in conjunction with the breast cancer awareness month of October 2021, this year we are having a project where we are focusing on caregivers. We are giving the platform to caregivers of metastatic breast cancer patients to narrate their experience and also to convey a message to the public and to other caregivers out there.
To find out more, surf to:
Sri Kota Specialist Medical Centre
Breast Cancer Welfare Association Malaysia